View & Print Insurance Card
Access your insurance card whenever you need it.
Prescription Drug Pricing Tool
Access current and complete drug pricing information.
View your Claims History
Check the status of your claim and view your claims history.
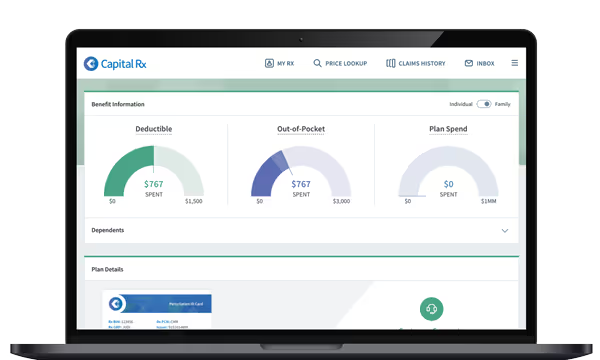
See Your Deductible & Out-of-Pocket Spend
Review your deductible and current spend for the year.
Check Drug Formulary Status
See the list of all covered drugs or search for a specific medication.
Access Member Materials
View and download the most current member materials.
Who is Capital Rx?

Capital Rx is a next generation pharmacy benefit manager, overseeing prescription benefit plans on behalf of employers, unions, and you- our members. We work hard every day to ensure your prescription plan is cost-effective while never losing sight of our ultimate mission: your health.
What is a pharmacy benefits manager (PBM)?

A pharmacy benefit manager (PBM) processes prescription drug claims on behalf of you and your plan sponsor (usually your employer, union, etc.). In order to provide this service, we contract and negotiate with retail pharmacies and pharmaceutical manufacturers to provide the right balance of drug access and cost-effectiveness.
Can I still fill my prescriptions at my preferred pharmacy with Capital Rx?

Capital Rx maintains a national network of more than 65,000 pharmacies, including all national chains and most independent pharmacies. However, with some prescription benefit plans, certain pharmacies may be excluded from the network. To confirm the network status of your preferred pharmacy, please log in to our member portal. Once you arrive at the pharmacy, don’t forget to show the pharmacist your ID card to ensure you only pay the out-of-pocket cost associated with your prescription benefit plan.
Is my current (or new) prescription covered by Capital Rx?

Your coverage for each prescription drug is outlined on our formulary (i.e. preferred drug list). Although most prescription benefit plans use our normal formulary, some plan sponsors require customization to best serve the needs of their membership. To confirm the coverage status of a medication- including if a prior authorization, step therapy, or quantity limit applies- please consult the formulary specific to your prescription benefit plan by logging into our member portal.
How do I know what my out-of-pocket cost (i.e. copay or coinsurance) will be?

What you pay for a prescription is determined by how your plan sponsor (usually your employer, union, etc.) has structured your prescription benefit. Although this information is not outlined on our formulary, you should have received a Summary Plan Document (SPD) or Schedule of Benefits during your most recent open enrollment period. This document will outline your out-of-pocket obligation for different types of medications (generics, preferred brands, non-preferred brands, specialty medications, etc.). Generics will almost always cost you (and your plan sponsor) less. Similarly, preferred brands are almost always cheaper for you (and your plan sponsor) than non-preferred brands. Please note: if your health plan has a deductible, you will be required to pay the full (discounted) cost of the medication until the deductible is met.
If you have additional questions, call us at (888) 832-2779.
How do I request reimbursement for a pharmacy claim?

If for any reason you were unable to apply your prescription benefit to fill a prescription, you can make a request for reimbursement by completing our direct member reimbursement form and mailing it to the below address, along with the original receipt from the pharmacy (please make a copy for your own records). Dependent on your plan's elections, you may be reimbursed directly for covered prescriptions.
Capital Rx
Attn: Claims Dept.
9450 SW Gemini Dr., #87234
Beaverton, OR 97008
Is mail order delivery right for me? If so, how do I enroll?

If you have a prescription for a maintenance medication (i.e. long-term conditions like arthritis, asthma, diabetes, high blood pressure, or high cholesterol), mail order delivery may be a great solution for you. First, mail order provides you with greater savings on most prescription benefit plans. Second, mail order saves you the time spent traveling to a retail pharmacy, waiting in line, etc. Third, mail order provides an easier way to complete refill requests. Some plans may require maintenance medications to be filled through mail order. To understand if this applies to you, please log in to our member portal.
For additional mail order questions, please call (888) 832-2779.
How do I check the status of my mail order prescriptions?

Mail order prescriptions are handled by Capital Rx’s contracted mail order pharmacy. For up-to-date information on the status of your mail-order prescription, please call us at (888) 832-2779.
What is a prior authorization (PA)?

A prior authorization (PA) is a feature of your prescription benefit plan that requires you and your physician to obtain approval before the prescribed medication can be dispensed by a retail or mail order pharmacy. This requirement exists to prevent inappropriate prescribing of certain medications and to ensure the lowest cost alternative is used (barring medical necessity). To submit a prior authorization (if required) please complete the prior authorization request form and fax it (along with any additional documentation required) to (833) 434-0563. Prior authorization request forms can also be sent via mail to the below address:
Download Prior Authorization Request Form
Capital Rx
Attn: Prior Authorization
9450 SW Gemini Dr., #87234
Beaverton, OR 97008
For additional prior authorization questions, please call (888) 832-2779.
How long does a prior authorization review take?

Most prior authorization reviews are completed within two business days provided that a complete prior authorization request form and all required documentation are correctly submitted. Our clinical team will notify you in advance of any declinations and assist in expediting your patient to a preferred alternative therapy.
What is a quantity limit (QL)?

A quantity limit (QL) is a feature of your prescription benefit plan that only allows you to receive up to a maximum dosage or quantity for certain medications (e.g. opioids). Quantity limit requirements exist to ensure safe and effective doses are prescribed and to prevent waste, fraud, and abuse. If you and your physician require a dose or quantity beyond what the quantity limit allows, please submit a prior authorization, including medical justification for the larger dose or quantity.
What is a step therapy (ST)?

A step therapy (ST) is a feature of your prescription benefit plan that requires you try another medication (usually a generic) before being prescribed the medication designated with step therapy (usually a brand). This requirement exists to prevent inappropriate prescribing of certain medications and to ensure the lowest cost alternative is used.
If your physician prescribes, or wants to prescribe, a medication designated with step therapy, please have them call us at (888) 832-2779
How do I replace a lost ID card?

To request a replacement Prescription ID card, please call us at (888) 832-2779. For immediate needs, please log in to our member portal, to view and print a temporary ID card.
What should I do if I'm traveling or on vacation and need immediate medication?

If you need additional assistance obtaining medication for extended periods of travel, please call us at (888) 832-2779.
How do I manage my member information on the Capital Rx portal? Can I use the member portal on my mobile phone?

To manage your member profile, please log in to our member portal. Our entire member site is mobile compatible.
What are the hours for Capital Rx's customer support line?

Our customer service representatives are available 24 hours a day, 7 days a week to answer any questions you may have about your prescription benefit plan. Your health is our priority. Please call us at (888) 832-2779 if you have any questions.
Can I request copies of information relevant to my claim?

Yes, you may request copies of the following (free of charge): All documents, records, clinical rationale or other information used in making the decision, the internal guideline or protocol relied upon in making this determination, any additional denial rationale or explanation of the decision, and if this determination is based upon medical necessity issues, experimental treatment issues or similar plan limitations, you or your authorized representative may obtain, upon request, an explanation about the scientific or clinical judgment for such determination. If you would like to receive any of the information described above, please contact us at:
Capital Rx
Attention: Appeals Department
9450 SW Gemini Dr., #87234
Beaverton, OR 97008
Phone: (888) 832-2779
Fax: (833) 434-0563